A healthy lifestyle and regular chiropractic care is a great foundation for keeping yourself well both mentally and physically. This is because chiropractic gets your nervous system functioning at its optimum. Particularly, when your autonomic nervous system is imbalanced you get symptoms such as high cortisol, high adrenalin, difficulty sleeping (insomnia), agitation, and anxiety most probably due to a hyperactive sympathetic nervous system. Moreover, if your neuroendocrine system (network of cells that produce and release hormones into the bloodstream) is not functioning at its optimum (e.g. due to diabetes, thyroid disease) it can make matters worse.
Chiropractic care and spinal manipulation regulate the autonomic nervous system at the peripheral level. And this regulation projects to your central nervous system. In particular, it may activate the parasympathetic system to counterbalance the activity of the sympathetic system. So your vagus nerve will be functioning at its optimum. Keep reading to find out about Exploring the Role of Chiropractic Care in Stress Relief and Emotional Health.
Your Nervous System
Firstly, your nervous system has a central nervous system and a peripheral nervous system. Secondly, the central nervous system is made up of the brain and spinal cord. Thirdly, the peripheral nervous system is made up of nerves that branch off from the spinal cord and extend to all parts of the body. Fourthly, your nervous system transmits signals between the brain and the rest of the body. Lastly, your nervous system’s activity controls the ability to move, breathe, see, think, and all functions to live.
Your Autonomic Nervous System
Your autonomic nervous system is a component of the peripheral nervous system that regulates involuntary physiologic processes. This includes heart rate, blood pressure, respiration, digestion, and sexual arousal. There are three anatomically distinct divisions: Sympathetic, parasympathetic, and enteric.

Sympathetic Nervous System (SNS)
Activation of the sympathetic nervous system leads to the “fight or flight” response. This response leads to a state of overall increased activity. Your blood pressure and heart rate will increase because your body is getting ready to physically react. Furthermore, glycogenolysis (release of glucose) occurs. This happens because you would require extra energy (glucose) for a “fight or flight” response. In contrast, gastrointestinal peristalsis (part of digestion) ceases.
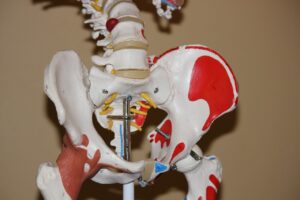
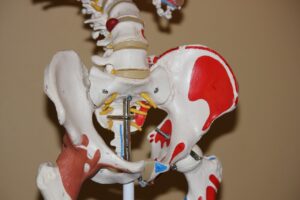
Your sympathetic nervous system innervates nearly every living tissue in your body. The origin of the sympathetic nervous system is found within the thoracic (mid) and lumbar (lower) segments of the spinal cord also known as the thoracolumbar division (T1 to L2).
Additionally, the following are more specific organ innervations (distributing of nerves for body function). Interestingly, it is said that the levels specified may be painful when the organ is involved (viscerosomatic pain):
- heart-C8-T5(T8)
- lungs-T3-T5(TIO)
- stomach-T5-T8(T9)
- pancreas-T7 -T9
- gallbladder, liver, spleen, caecum, and duodenum-T6-TIO
- appendix- T9-Tll
- kidneys- T9- L2
Parasympathetic Nervous System (PNS)
In the opposite way, your parasympathetic nervous system promotes the “rest and digest” processes. Your heart rate and blood pressure lower, gastrointestinal peristalsis/digestion restarts, etc. The PNS is significantly smaller than the SNS. It innervates only the head, viscera (organs), and external genitalia. Notably, the PNS is vacant in much of the musculoskeletal system and skin.
The parasympathetic system originates from cranial nerves III, VII, IX, and X as well as sacral levels S2–4. While the sympathetic chain synapses closer to the spinal cord, the parasympathetic synapses at the target organ. A synapse is a junction between two nerve cells, consisting of a minute gap across which impulses (electrical signal traveling along the axon of a nerve cell) pass.
The Enteric Nervous System
The enteric nervous system (ENS), also known as the intrinsic nervous system, controls the gastrointestinal tract. It contains complete reflex neural circuits that detect the physiological condition of the gastrointestinal tract. Next it integrates information about the state of the gastrointestinal tract, and provides outputs to control gut movement, fluid exchange between the gut and its lumen, and local blood flow.
It is the only part of the peripheral nervous system that contains extensive neural circuits. Your ENS is capable of functioning independently of the remainder of the nervous system. Because of the extent of autonomy, the ENS has been called a second brain. Of course, the ENS has extensive, two-way, connections with the central nervous system (CNS). Similarly, the ENS works along with the CNS to control the digestive system for your body’s physiological demands.
The Vagus Nerve
The vagus nerve, cranial nerve X (CN 10), makes up about 75% of the PNS and provides parasympathetic input to most of the thoracic and abdominal viscera, with the sacral parasympathetic fibers innervating the descending and sigmoid colon and rectum. The vagus nerve arises from four nuclei (clusters of brain cells) in the brainstem: the dorsal motor nucleus, the solitary tract nucleus, the spinal trigeminal nucleus, the nucleus ambiguous.
Your vagus nerve is the longest and most complex of the cranial nerves.
The vagus nerve runs from the brain through the face and thorax to the abdomen. It is a mixed nerve. The vagus nerve has sensory ganglia (masses of nerve tissue that transmit sensory impulses) innervating the skin in the concha (middle external) of the ear. So the vagus also gives off cardiac, esophageal, and pulmonary branches. In the abdomen the vagus innervates the greater part of the digestive tract and other abdominal viscera.
Indeed, the vagus nerve has the most extensive distribution of all the cranial nerves. For instance, its pharyngeal and laryngeal branches transmit motor impulses to the pharynx (throat) and larynx (voice box). Secondly, its cardiac branches act to slow the rate of heartbeat. Thirdly, its bronchial branch acts to constrict the bronchi. Fourthly, its esophageal branches control involuntary muscles in the esophagus, stomach, gallbladder, pancreas, and small intestine, stimulating peristalsis and gastrointestinal secretions.

Why Chiropractic Adjustments Can Correct Sympathetic /Autonomic nervous system Dysfunction
Chiropractic Subluxations (Misalignments) in your spine can cause neurodysfunction. It can potentially cause direct mechanical irritation of your Sympathetic nervous system. This model is based on the anatomic closeness and vulnerability of the posterior chain ganglion (masses of nerve tissue) between T1 and L2 (thoracic level 1 to lumbar level 2) to the posterior (further back) chest wall and costovertebral joints (joints that connect the ribs to the spinal vertebral column). This is part of your sympathetic chain which is located bilaterally (both sides) to your spine. The sympathetic chain extends from the base of the skull to the coccyx.
In conclusion, altered spinal and costovertebral mechanics are hypothesized to irritate the sympathetic ganglia. In turn, this induces segmental sympathetic “hypertonia” (increased tone). The target organs within the segmental distribution are then theoretically affected. The outcome is the organs have dysfunction in autonomic regulation and function as a result of altered sympathetic function.
Why Chiropractic Adjustments Can Correct Autonomic Dysfunction: Parasympathetic Nervous System (PNS)
In contrast to the sympathetic chain, the parasympathetic system, with its origins in the brain, brainstem, and sacral segments of the spinal cord, does not have anatomic proximity to the spinal joints. Models of mechanically induced dysfunction of the parasympathetic system have dysfunction in cranial (head), cervical (neck), and pelvic (pelvis) mechanics as potential sources of entrapment or tethering of the parasympathetic fibers. Altered cervical, cranial, or cranio-sacral mechanics are likely to induce traction of dural attachments and the cranial nerves as they exit through the dura (membane surrounding brain and spinal cord) and skull foramina (opening in skull). Indeed, the parasympathetic nervous system regulates the upper cervical (neck) region. So a cervical or cranial manipulation/adjustment results in a parasympathetic response (lowering of heart beat, reduction of blood pressure, pupil constriction).
Exploring the Role of Chiropractic Care in Stress Relief and Emotional Health
In one research study, scientists found Chiropractic and spinal manipulative therapies along with vagal nerve stimulation may therefore be regarded as treatment options for depression (2).
The chiropractic treatment goal in mechanically induced autonomic dysfunction is to identify the sites of joint dysfunction and apply appropriate manual therapy to balance tension/misalignments.
Chiropractic therapy works on the nervous system, stimulating it to release various chemicals and hormones that regulate blood pressure and flow, calm the brain and reduce inflammation. Many studies have explored chiropractic cranial and vertebral adjustments, and spinal manipulative therapy in relation to autonomic functions. In conclusion, chiropractic adjustments may improve autonomic imbalance.
In conclusion, chiropractors focus on the evaluation and treatment of neuromusculoskeletal (NMS)-based disorders. However, chiropractors also help treat the multiple potential causes of ill health including chronic stress and your emotional health/wellness. The chiropractor holistically views the human being as a dynamic, integrated, and complex living being who has an innate capacity for self-healing. Successfully reduce your stress and its consequences with natural chiropractic care!
Do you know anyone who would benefit from chiropractic care? Call your chiropractor serving West Palm Beach, Jupiter, North Palm Beach, Palm Beach Gardens and the surrounding areas at 561-253-8984 to make an appointment or to learn more about Exploring the Role of Chiropractic Care in Stress Relief and Emotional Health .
References:
(1) Thomas Souza, (2018) Differential Diagnosis and Management for the Chiropractor
(2) https://pmc.ncbi.nlm.nih.gov/articles/PMC8023121/
(3) Bergman, Thomas. Peterson, Lawrence. Chiropractic Technique Principles and Procedures 2011. Third Edition