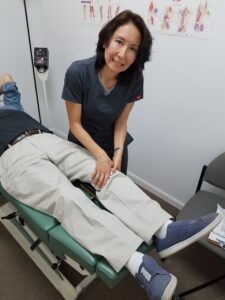
Do you have persistent pain, burning, aching, or numbness in the back side of your leg, ankle, or foot? These are all symptoms of Sural Neuropathy. Read on to learn about Ankle and Foot Pain Due to Sural Neuropathy: Chiropractic Can Help.
Anatomy of the Sural Nerve
The sural nerve is a cutaneous (affecting the skin) nerve. So it is purely sensory. It provides only sensation to the posterolateral (back outside) aspect of the distal (away from body) third of the leg and the lateral (outside) aspect of the foot, heel, and ankle.
It is formed by terminal (ending) branches of the tibial and common peroneal nerves (both branches of the sciatic nerve) that join together in the distal third of the leg.
The Sural Nerve descends between the two heads of the gastrocnemius (calf muscle). Next, it pierces the deep fascia (casing of connective tissue holding muscles) in the middle or upper part of the back of the leg. Then it is joined by the sural communicating branch of the common peroneal nerve. Finally, it continues to the lateral malleolus (bump of bone on the outside of your ankle).

Entrapment Sites
Sural nerve entrapment/neuropathy most commonly occurs in the ankle/foot area. The entrapment site located approximately two thirds the distance between the knee and the heel is a less common entrapment location. The most common sites are in the fascia just above the ankle and behind the lateral malleolus.
Sural Neuropathy/Nerve Entrapment Causes
Your pain and paresthesias (numbness and tingling) could have come on insidiously (gradually). However, Sural neuropathy/nerve entrapment can be due to various causes such as trauma, bakers cyst, scaring, fascial restrictions and vascular problems.
Firstly, tight boots and lacing may be the cause of compression of the sural nerve.
Secondly, different forms of trauma can be a leading cause of sural nerve pain. For instance after an ankle sprain or an ankle fracture. Afterwards, this can create significant pulling and traction on the nerve. Additionally, direct impact to the nerve from being kicked, falling, or an accident can be a cause.
Thirdly, entrapment sites are areas along the nerve’s pathway that may become entrapped, causing more pressure on the nerve. For instance, like carpal tunnel syndrome in the hand.
Fourthly, trauma from surgery can cause sural neuropathy. Sadly, this may be a common cause of chronic pain CRPS (Complex regional pain syndrome). And this is often in the news because of the American opiate crisis. Patients are taking harmful drugs due to pain. And some of these patients’ pain could be related to this painful sural neuropathy. Various surgeries in the ankle, foot and leg can injure the sural nerve, resulting in sural nerve pain.
Here are some examples of Sural Neuropathy after surgery:
- Heel Fractures: Surgey is performed on the outer side of the heel bone which is next to the pathway of the nerve. A post-surgical scar can occur which irritates the nerve. So the nerve can become entrapped and tangled in the scar.
- Achilles Tendon Repair: Similarly, surgery performed on the achilles tendon for repair or lengthening places the nerve at a risk for injury.
- Ankle Surgery: Any ankle surgery may also cause injury to the nerve.
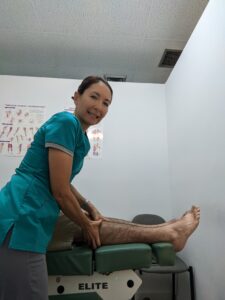
Treatment at Meiri Chiropractic for Sural Neuropathy
First, soft tissue techniques will be rendered to the contracted fibrotic muscle and collagen at entrapment sites.
Second, chiropractic adjustments (chiropractic manipulative therapy) to the foot, ankle and associated restricted joints along the kinetic chain is important.
Third, therapeutic exercise will be given for stretching and strengthening.
Lastly, if trauma or swelling is involved, ice, compression, elevation, and physical therapy modalities is utilized to reduce swelling. Also, an orthotic and/or correction of shoes may be necessary.
Are your suffering from leg, ankle or foot pain from Sural Neuropathy?
We offer excellent Chiropractic care for Sural Neuropathy. At Meiri Chiropractic, we spend the time necessary to examine, diagnose and treat every neuromusculoskeletal condition and various ailments you have. Indeed, Chiropractic is a holistic and natural way to not only treat leg, foot and ankle pain, but to keep your body in its best working condition. We have been offering effective chiropractic care in West Palm Beach since 2006. Many of our patients reviews note our excellence. Call us today at 561-253-8984 to make an appointment or to find out more about Ankle and Foot Pain from Sural Neuropathy: Chiropractic Can Help.