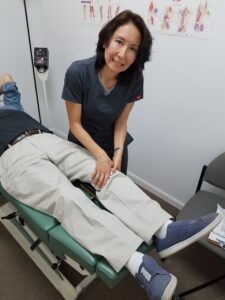
Many people dealing with Multiple Sclerosis (M.S.) feel as though they have very few options for managing their pain. Chiropractic care maybe the answer!
In one study (1), manual chiropractic adjustive therapies appear to be responsible for the dramatic symptomatic relief provided for a patient diagnosed with M.S. Consequently, it was concluded “the relative risk-to-benefit ratio suggests that this approach may be appropriate as an alternative symptom management approach for MS”.
What is Multiple Sclerosis (M.S.)?
Typically, M.S. patients are less than 55. And it is more prevalent in women than men. MS appears in patients who reside in temperate climate zones and are of western European ethnicity. Relapses commonly occur in women 2 to 3 months after childbirth.
MS is characterized by episodic attacks that initially resolve, but eventually leave residual neurologic deficits. The initial episode often will resolve in days. Next, the patient may remain symptom free for months or years. Eventually, however, symptoms recur. Symptoms usually will involve a region and consist of numbness, tingling, weakness, diplopia (double vision), dizziness, or urinary sphincter dysfunction (urgency or hesitancy).
Cause
The cause of MS is unknown, but scientists think it may be an immune disorder (condition in which the body attacks itself by mistake).
There is an apparent genetic relationship due to the association of MS and HLA-DR2. The human leukocyte antigen (HLA) is a family of genes found on chromosome 6 which provide the instructions to make a group of proteins known as the HLA complex. The HLA proteins are present on the surface of cells, and they help the immune system to distinguish foreign invaders such as viruses and bacteria from the body’s own cells and tissues.
The primary role of the HLA complex is in the regulation of the immune system to defend against disease. Your individual HLA type is inherited from your parents. In MS, the immune system fails to distinguish between the body’s tissues and foreign proteins. This results in your body attacking your own central nervous system.
Demyelination
Firstly, MS attacks myelin as if it were foreign. And Myelin is an insulating layer, or sheath that forms around nerves, including those in the brain and spinal cord. Secondly, MS is a disease characterized by patchy demyelination with reactive gliosis. Gliosis is a process leading to scars in the central nervous system that involves the production of a dense fibrous network of neuroglia (supporting cells) in areas of damage. Thirdly, this occurs in the spinal cord, optic nerve (nerve for transmitting visual images), and white matter of the brain. Lastly, Gliosis is a prominent feature of many diseases of the central nervous system, including multiple sclerosis and stroke.
Diagnosis and Findings on Imaging
No single test can diagnose MS. The medical history, neurologic exam and lab tests helps rule out other diseases and confirm MS. For example, Laboratory evaluation may reveal mild lymphocytosis (increased white blood cells) or increased protein count in the cerebrospinal fluid (CSF). Immunoglobulm G (type of antibody) are more often seen in the CSF.
Furthermore, Magnetic Resonance Imaging (MRI) will demonstrate multifocal areas of patchy demyelination in the brain or cervical (neck) spinal cord.

Management of Multiple Sclerosis
First, there is no cure for MS.
Second, natural Nutritional approaches may help, but there is not enough research. Some studies suggest that an increase in polyunsaturated fatty acids and metabolic enzyme supplements help. This nutritional supplementation may assist in providing an adequate lipid pool for oligodentrocytes (cell concerned with the production of myelin in the central nervous system). Also, antioxidants such as vitamins A, beta-carotene, E, C with bioflavinoids, and selenium may help with myelin membrane perioxidation (free radical reaction).
Third, chiropractic is a popular CAM (complementary alternative medicine) therapy for symptom relief of M.S. In one study, conservative chiropractic manual adjustive therapies were provided to address spinal segmental dysfunction. And the patient reported complete absence of symptoms following the first treatment intervention.
Are you seeking a natural treatment to help relieve Multiple Sclerosis (MS) symptoms? Your chiropractor in West Palm Beach can help you manage your symptoms and improve your overall quality of life. Call 561-253-8984 today to make an appointment or to find out more about Chiropractic Care in West Palm Beach: Multiple Sclerosis Pain Relief.